The current obesity epidemic is really an epidemic among men, said John La Puma, MD, at Holistic Primary Care’s fifth annual Heal Thy Practice conference in Long Beach earlier this month. 
Women tend to be the focus of much of the public and clinical attention on weight problems—presumably because women are more likely to seek care, and social norms pressure women to be thin. But overweight is actually more common among men, said Dr. La Puma, author of the forthcoming book, Men Don’t Diet, Men…Refuel.
“There’s a lot more illness among men, and a lot less healthcare,” he said. Incidence of obesity in women has been steady over the last decade while in men it has increased. From 2000 to 2008, median BMI for women was at roughly 27 (Flegal KM, et al. JAMA 2010; 303: 235-241). In men, it rose from roughly 26 to 30. Currently, 72% of American men are overweight or obese versus 64% of women.
Calling it the “other gender gap,” Dr. La Puma said, “Men are asleep at the wheel of their health.”
It’s easy to point the finger at poor diet and sedentary living. But Dr. La Puma says there’s more to the picture than beer, burgers & Breaking Bad.
Other, less obvious factors are also adversely impacting male metabolism.
The Other Gender Gap
In many ways, men are far less healthy than women.
Average US life expectancy is 76 years for men versus 81 for women. Lifetime cancer risk is 50% for men versus 33% for women. As of 2006, 6% of all US males had been diagnosed with T2D, compared with 5.5% of women. Both numbers are markedly increased from under 3% in the late 1980s, and there’s no reason to think the trend has slowed down in the 7 years since those figures were published.
Coronary heart disease is the number one killer of both men and women in America, but mortality starts at much younger ages in men. Dr. La Puma noted that between the ages of 45-65, men average approximately 265,000 new and recurrent myocardial infarctrions or fatal CHD events compared with only 95,000 in women. In the 65-74 bracket, there were 180,000 new cases among men and 95,000 in women.
Women’s CVD event & death rates only reach parity with men’s after age 75.
It’s no big secret that men are less likely to seek medical attention, but on a population basis, the numbers are quite alarming.
According to CDC data from 2007, the number of men who’d never been to a doctor in the previous year was 23% versus 12% of women. At the other end of the utilization spectrum, the number of men who’d had 10 or more visits to a physician or hospital was 10% versus 15% for women (CDC: Trends in the Health of Americans, 2007).
Given the protracted recession, the high unemployment rates, and the number of people who have lost their healthcare insurance over the past 6 years, the disparity pattern has probably gotten worse since those data were published.
The T-cline of Civilization?
Dr. La Puma holds that these morbidity and mortality patterns are connected to three inter-related factors: declining testosterone, increasing visceral fat deposition, and chronic inflammation.
Testosterone, like many other hormones in both males and females, tends to decline with age. By age 45, testosterone production slows down in most men, and by age 60, a man’s total testosterone level is considerably lower than it was in his 40s. No big surprise there.
But what IS surprising is the fact that at all age points, men today have lower average testosterone levels than their predecessors.
In a landmark prospective study published in 2006, Thomas Travison and colleagues at the New England Research Institutes reported on total serum and free testosterone levels from three large cohorts of Boston-area men, aged 45-79 years. The cohorts represented distinct data collection “waves” separated in time by several years. The first group was tracked from 1987 to 1999, the second from 1995-1997, and the third from 2002-2004.
They found, “a substantial age-independent decline in T that does not appear to be attributable to observed changes in explanatory factors, including health and lifestyle characteristics such as smoking and obesity.”
Further, the authors note that these population-level declines are greater in magnitude than the expected testosterone declines typically associated with aging (Travison T, et al. J Clin Endocrinol Metab. 2007; 92(1) 196-202).
Dr. La Puma emphasized that this is by no means a local phenomenon. Similar patterns have been shown in populations across the globe. “There’s been a worldwide testosterone decline.”
Sperm counts are also declining. In 2007, an alarming report from the University of California San Francisco entitled Shaping Our Legacy: Reproductive Health & the Environment, indicated that average sperm counts had dropped by 50% over the last 50 years. At the same time, 46% more men are getting testicular cancer, and 76% more men are getting prostate cancer.
The pan-global “sperm crisis” was the subject of a contentious day-long debate at last summer’s meeting of the European Society of Human Reproduction & Endocrinology (ESHRE), and was covered in the Wall Street Journal and other media outlets. Among the headline-grabbing findings was a French study showing a 33% decline in sperm concentration among French men from 1989 to 2005.
An Estrogen Factory
Declining testosterone, increased insulin resistance and weight gain in men are all strongly associated with deposition of visceral fat, a phenomenon that is increasingly recognized as a primary factor in the pathophysiology of many disorders in men.
Overweight men are nine times more likely to have low testosterone than those who are not overweight.
Insulin sensitivity shows a strong inverse relationship with visceral fat as a percentage of total body weight. This was well-documented in women 1996 by Carey and colleagues, who showed that those with BMIs greater than 25 were much more likely to be insulin-resistant than those with BMIs under 25. Presumably a similar relationship holds in men as well, and it is arguably more dangerous in males.
Visceral fat is, more or less, an estrogen factory, converting testosterone to estrogen leading to further fat deposition and greater metabolic dysregulation. It is, says Dr. La Puma, a primary factor in the declining testosterone levels seen in industrialized nations.
To condense all the physiology down into terms most guys will understand, Dr. La Puma poses a sharp question: Is your belly turning you into a girl?
Poor diet is a contributor to the problem, but it is not the only one. Dr. La Puma contends that environmental toxins, pesticide residues and drug metabolites also play a major role in estrogenizing men.
Industrial Toxins
“Atrazine, Bisphenol-A (BPA), DDT, DES Phthalates, PCBs are all hormonally active. These are every day chemicals that are widely used and highly prevalent in our lives.”
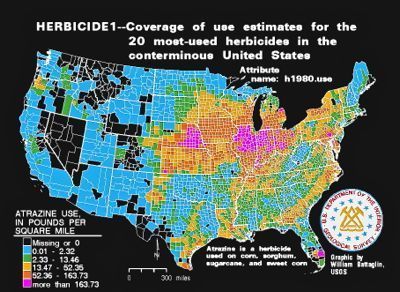 Many people do not realize that there are upwards of 75 million pounds of Atrazine herbicide—an androgen antagonist–pumped into earth every year to produce corn. “It leaks out into the water supply, and has spread from the Midwest to New England, down into south, and it spreads west only stopping the continental divide.”
Many people do not realize that there are upwards of 75 million pounds of Atrazine herbicide—an androgen antagonist–pumped into earth every year to produce corn. “It leaks out into the water supply, and has spread from the Midwest to New England, down into south, and it spreads west only stopping the continental divide.”
Comparing a map of atrazine use with one showing obesity trends, there’s a marked and disturbing geographic overlap.
Pthalates, another common estrogenic chemical found in paints and plastics is associated with increased waist circumference and lower fertility in men, as well as obesity in children. BPA is found in coated papers, on the inside of cans and in many plastic bottles and containers, is another common estrogen 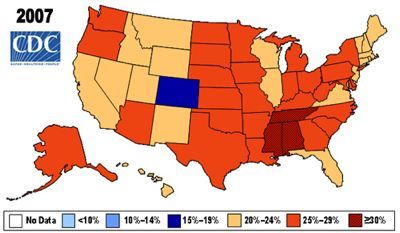 mimic.
mimic.
TRT Time?
Given the high prevalence of both obesity and low testosterone, it’s no surprise that use of testosterone replacement therapy (TRT). Since 2001, the number of TRT prescriptions has tripled. Last year, TRT racked up $2 billion in sales, and could hit $4 billion by 2017.
“Doctors are prescribing T for erectile dysfunction, but it doesn’t work well for that,” said Dr. La Puma, adding that in roughly one-third of all men who get TRT from walk-in clinics, nobody has even measured their testosterone levels.
This, he says, is a dangerous trend, because TRT is not without risks. Known adverse effects include: thickening of blood clots, reduced sperm count, liver problems, male pattern baldness, acne, higher risk of CVD, and gynecomastia. Further, transdermal testosterone—the most common mode of TRT delivery–can rub off on the user’s family members or partners.
Some researchers have suggested that TRT increases the risk of prostate cancer. While that’s not been definitively proven, Dr. La Puma says it’s certainly plausible, and worth considering.
The bottom line is that TRT needs to be used far more judiciously; it is only appropriate for men with documented low testosterone levels.
The reality is that lifestyle changes are much more effective in maintaining testosterone, regulating weight, improving glucose metabolism, and reversing risk of serious disease.
Dr. La Puma noted that men who eat healthfully and exercise regularly typically sustain their mid-life testosterone levels well into their 60s and 70s. The age-associated declines are not necessarily inevitable, nor are they irreversible.
The Refuel program which Dr. La Puma has been developing with his patients over the past few years provides a comprehensive blueprint for helping men make and sustain meaningful diet and lifestyle changes. It’s packed with recipes—Dr. La Puma is also a trained chef and wine expert—and tailored to hit the “reward” circuits in mens’ brains.
Success and pleasure, he says, are much better long-term motivators than fear, privation and nagging.
Here are some of his tips for helping men grab hold of the steering wheel of their own health.
The CYCYP Test: Nothing quite makes the point about visceral fat like having a man look up, then look straight down, and asking, “Can you see your penis?” An answer of “No,” will likely provide way more motivation than a battery of biomarkers and lipid measures.
Eat Crucifers: “This is evidence-based medicine!” says Dr. La Puma. Cruciferous veggies like Brussels sprouts, watercress, kale, mustard greens, cauliflower, broccoli, and daikon are packed with glucobrassin and other sulfur compounds that convert estrogen to its least estrogenic forms. Steaming is the best mode of preparation.
Add Vitamin D: This vitamin lowers sex hormone binding globulin (SHBG). In one study, men who had D levels under 40, showed a 10% increase in total testosterone following supplementation that raised serum D levels over 50. If men are vitamin D-deficient they will show a testosterone rise after 3,000 units. “I start with 1,000 units per day. I’m conservative,” Dr. La Puma said.
Eat More Mono-unsaturated Fats: Avocados, olives & olive oil, nuts and nut oils are extremely healthy, because mono-unsaturated fats help Leydig cells transport cholesterol increase manufacture of testosterone. The leydig cells need adequate circulating unsaturated fats to make testosterone, which is why men on very low fat diets (<30% fat) show lower T levels than those on higher fat diets.
Cut Carbs Twice Weekly: Carving out the carbs forever is not a feasible option for most guys. But the vast majority can handle a major carb-cut every few days. Dr. La Puma recommends that patients commit to eating no more than 50 grams of carbs twice weekly. On other days, they can eat carbs freely (within reason of course). This pattern, which most guys can embrace, simulates the alternating cycles of caloric plenty & poverty that our paleo ancestors faced.
Use Six-Inch Plates: Visual cues play a major role in eating habits. Smaller plates make portions look bigger, and can help prevent over-eating.
Squat, Don’t Run: Running is not an efficient way to burn visceral fat. Squats, pushups, Burpees and jumping jacks are far better. Dr. La Puma recommends quick cycles of 10-second high-intensity bursts several times per day. “We do this with guys who are not at all fit. It gets them going and puts points on the board right away.”
Avoid Plastics: Make men aware that many forms of plastic contain estrogenic compounds. Whenever possible avoid plastic food containers and bottles, and seek out Phthalate-free and BPA-free containers. Never heat plastics, as heat will cause the release of toxins. That means no microwaving food containers.
END







