Chronic stress can wreak havoc on the body, and emerging field of human social genomics is illuminating the mechanisms.
Conventional medical thinking often marginalizes psychosocial stressors as “soft” variables, less important than measurable biochemical markers of disease. But the fact is that stress can directly affect the ways in which our genes express themselves.
Recent findings indicate that a host of social-environmental conditions including poverty, major difficult life events, and social isolation can significantly alter genome expression. Likewise, certain behavioral factors have the power to alter genetic expression (Cole, S. PLoS Genet. 2014; 10(8): e1004601).
Typically, we experience our bodies as being biologically stable, since, from moment to moment, we cannot sense shifts in the functionality of our genes.
 But human social genomics researchers have found that stressful experiences — even if they’re relatively short — can influence the operation of hundreds of different genes at any given time, causing some genes to turn on and others to turn off. While many of these genetic changes are adaptive, some can be harmful — particularly when they’re prolonged due to ongoing stress or anxiety.
But human social genomics researchers have found that stressful experiences — even if they’re relatively short — can influence the operation of hundreds of different genes at any given time, causing some genes to turn on and others to turn off. While many of these genetic changes are adaptive, some can be harmful — particularly when they’re prolonged due to ongoing stress or anxiety.
“This is why it is critical to assess the amount of stress that all patients are experiencing,” says George Slavich, PhD, clinical psychologist and Director of the Laboratory for Stress Assessment and Research at the University of California, Los Angeles. Slavich has spent the past eight years developing the Stress and Adversity Inventory (STRAIN), a novel online system for assessing an individual’s lifetime exposure to stress.
“Assessing patients’ stress levels with the STRAIN is important for providers who treat patients experiencing a wide variety of different mental and physical health problems that can be influenced by stress, including anxiety, depression, asthma, arthritis, chronic pain, irritable bowel syndrome, autoimmune disorders, heart disease, and certain types of cancer,” Slavich argues.
While not all of these conditions result directly from stress, they can all be worsened by it, underlining the importance of stress management and reduction as critical treatment targets among at-risk patient groups.
Wide Variety of Biological “Selves”
Studies by Slavich and others in this emerging field point to stress-related changes in genome function as key drivers of human health and behavior. The discoveries challenge the long-held perspective that our “molecular selves” are fixed across time and situations. Instead, it appears that the genome can encode “a wide variety of ‘potential biological selves.’ “
Which “biological self” becomes expressed appears to result from the social conditions we experience throughout our lives (Slavich, G. & Cole, S. Clin Psychol Sci. 2013; 1(3): 331–348).
Intense toxic stress contributes to an excessive activation of stress hormones, which can damage the metabolic, cardiovascular, immune, and nervous systems and influence the etiology of various chronic diseases (Gilbert, L. et al. Am J Prev Med. 2015; 48(3): 345-349).
One group of investigators identified 209 genes that were differentially expressed between individuals who reported high versus low social isolation. People experiencing chronically high levels of social isolation are at elevated risk of inflammatory disease, identifying among them a unique tendency towards immunological activation.
When compared with more socially engaged individuals, the immune cells of socially isolated people showed an increased expression of genes controlling basic cellular transcription processes, cell cycle progression, pro-inflammatory cytokine signaling, and prostaglandin synthesis. The researchers note that this pattern of immune cell transcriptional dynamics heightens the risk of inflammation-mediated disease, impairs their humoral immune responsiveness, and decreases their ability to fight viral infections, making them more vulnerable both to infections like the common cold as well as a host of chronic conditions marked by inflammation (Cole, S. et al. Genome Biol. 2007; 8(9): R189).
Other studies indicate that social adversity like low socio-economic status, social rejection, and ongoing interpersonal difficulties can also 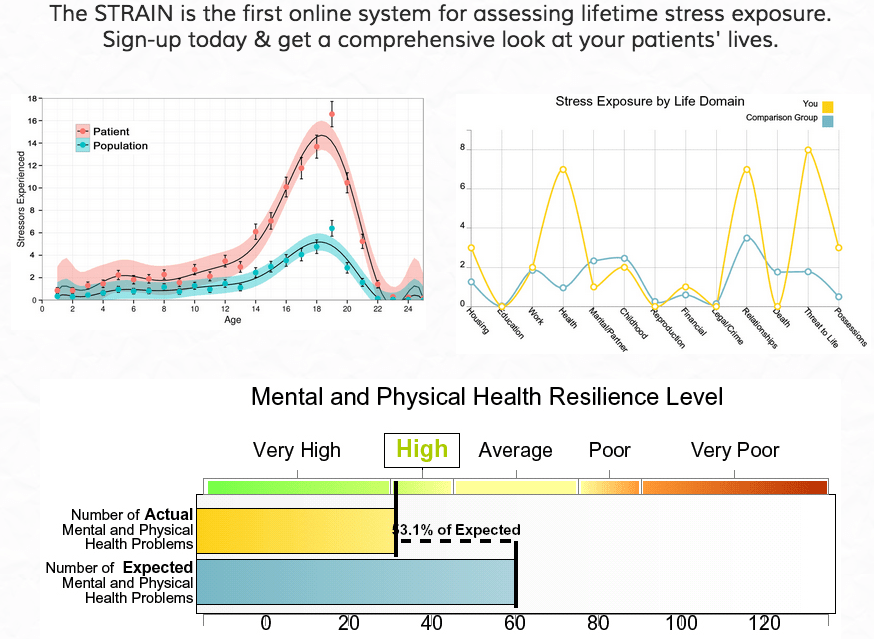 influence the expression of our genes, similarly skewing the the basal transcriptome in white blood cells towards a more pro-inflammatory, anti-antiviral state.
influence the expression of our genes, similarly skewing the the basal transcriptome in white blood cells towards a more pro-inflammatory, anti-antiviral state.
Assessing the “Environome”
There are a variety of psychological wellbeing scales that can aid practitioners in analyzing their patients’ stress levels. However, most existing assessment tools are not able to predict the biological processes that we now know deeply affect human health. Additionally, none of them account for stress as it occurs throughout the entire life course.
These two shortcomings led Slavich to the creation of STRAIN. The tool is designed to shed light on the specific stress-related forces that can cause patients’ genomes to shift in a more inflammatory direction.
STRAIN is a secure, easy-to-use online protocol for assessing an individual’s “environome.” It does so in a relatively quick, low-cost, and reliable manner. STRAIN analyzes nearly 100 different acute life events and chronic difficulties that a patient may experience throughout his or her lifetime.
Based on the information it collects, the assessment generates up to 15 different life stress summary scores and life charts depicting each patient’s individual exposure to acute, chronic, and overall life stress. It also calculates several stress resilience scores that help practitioners and patients identify strengths and levels of resistance to stress.
STRAIN takes about 25 minutes to complete online. The system generates a PDF version of the report that can be instantly emailed to patients and their practitioners.
Clinics that use STRAIN are provided with secure test website links unique to those clinics. Once setup to run the assessment, practitioners can ask patients to complete the test either at home before an office visit or on-site at a healthcare facility.
Dr. Slavich says patients really benefit from guidance from a health expert when trying to interpret the ways in which their personal stress levels impact their psychological and physical health status. The process opens the door to an ongoing dialogue around individually-tailored stress management treatment planning.
The “patient-provider exchange gives providers the opportunity to tell patients about adjunctive stress reduction classes or stress management strategies that might be helpful,” Slavich adds.
He aims to make the STRAIN available to all practitioners and clinics interested in improving their patients’ health by attenuating the detrimental genetic and physiological effects of psychosocial stress.
Additional information about the STRAIN is available online at http://www.expertstresstest.com.
END







