 Wildfires and tsunamis. Droughts and floods. Species die-offs and infectious disease outbreaks. Chemical spills and critical habitat destruction. Ocean acidification and coastal erosion. Hardly a day goes by without news of another climate-related disaster somewhere in the world.
Wildfires and tsunamis. Droughts and floods. Species die-offs and infectious disease outbreaks. Chemical spills and critical habitat destruction. Ocean acidification and coastal erosion. Hardly a day goes by without news of another climate-related disaster somewhere in the world.
The scale and frequency of these events—and the public outcry about them—are difficult to ignore, especially with millions of young people worldwide taking to the streets.
Environmental issues are usually framed in political, economic, and social terms. Lately, though, medical professionals are waking up and demanding that global warming be treated as a public health crisis.
There have always been medical voices calling attention to the perils of unchecked environmental degradation, but for the most part the healthcare mainstream has kept quiet. It is only recently that major medical organizations have begun to publicly acknowledge the health risks posed by climate change.
A Moral Imperative
Earlier this year, Caren Solomon, MD, MPH of Harvard Medical School and Regina LaRocque, MD, MPH of Massachusetts General Hospital, published a perspective article in the New England Journal of Medicine entitled “Climate Change––A Health Emergency” (Solomon, C. & LaRocque, R. N Engl J Med. 2019; 380: 209-211).
“Disruption of our climate system, once a theoretical concern, is now occurring in plain view—with a growing human toll brought by powerful storms, flooding, droughts, wildfires, and rising numbers of insect-borne diseases,” they wrote.
Solomon, an internist, and LaRocque, an infectious disease specialist, argue that, “Physicians are well placed and, we believe, morally bound to take a lead role in confronting climate change with the urgency that it demands.” They readily admit that the issues are overwhelming.
LaRocque and Solomon are among a growing cadre of clinicians at renowned institutions calling attention to the relationship between global warming and human illness––and calling on clinicians to take action.
“The Greatest Challenge”
Nobody says it is going to be easy.
The World Health Organization (WHO) describes climate change as “the greatest challenge of the 21st century, threatening human health and development.”
development.”
“The longer we delay action, the greater the risks to human lives and health,” WHO warns, a position the organization has held for several years. In 2015, it called for a “strong and effective climate agreement that will save lives, both now and in the future.”
“The evidence is overwhelming: climate change endangers human health,” said then WHO Director-General Dr. Margaret Chan.
More recently, a consortium of over 70 medical groups including the American Medical Association, the American Association of Family Physicians, The American Academy of Pediatrics, the American College of Physicians, and the Academy of Integrative Health & Medicine, issued an historic call to action, defining the climate crisis as “one of the greatest threats to health America has ever faced.”
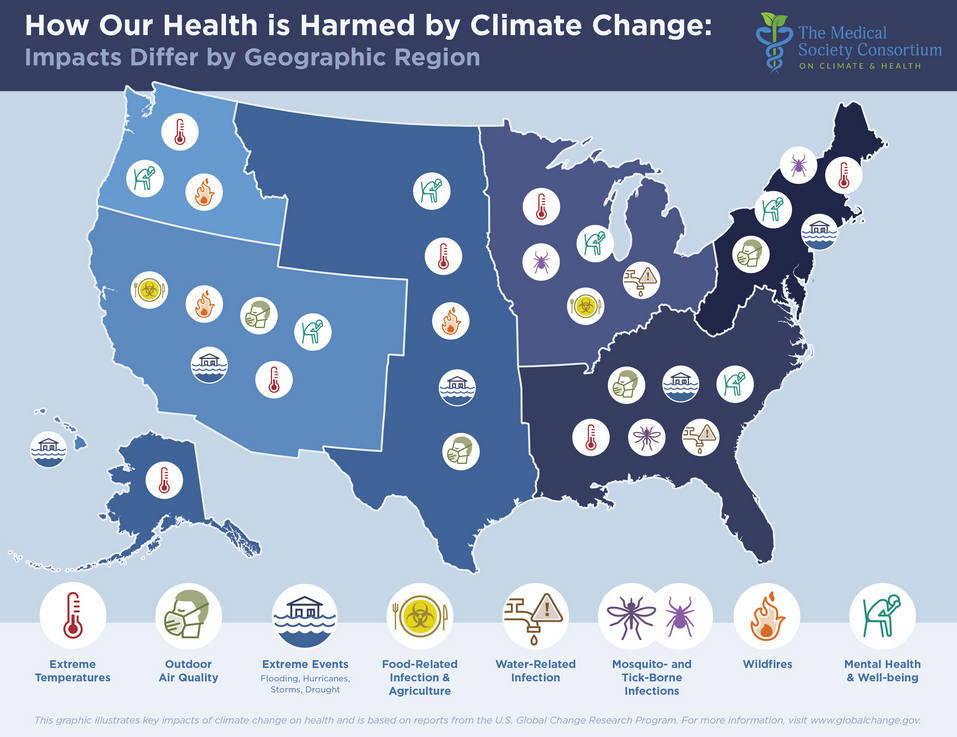
The authors cite extreme heat, massive storms and floods, year-round wild fires, air pollution, mosquito- and tick-borne diseases, and contamination of municipal water supplies. All are on the rise across the US. While none of these problems is new, they are all occurring more frequently and more widely, resulting in greater numbers of deaths, hospitalizations, and long-term disabilities.
As with so many other social problems, the fallout of climate dysregulation ends up in physicians’ offices, emergency departments, and hospitals.
The consortium produced the Climate, Health and Equity Policy Action Agenda urging government officials, policymakers, businesses, and civic leaders to prioritize a core set of climate-related actions including:
- Transitioning away from oil, coal, and natural gas and phasing out investments in and subsidies for fossil fuels, while encouraging use of renewable energy sources;
- Reducing greenhouse gas emissions across all industries;
- Encouraging active forms of transportation (bicycling, walking) and use of public transport while minimizing dependence on automobiles;
- Supporting investments in zero carbon emission vehicles and other green tech;
- Expanding public green spaces, parks, and forests;
- Minimizing food waste and promoting agricultural practices that increase carbon sequestration;
- Promoting plant-based diets and reduction of meat consumption;
- Advocating for access to safe, affordable drinking water for all;
- Widespread adoption of smart energy, waste reduction, and low-carbon technology throughout hospitals and healthcare clinics
“A just transition to clean, safe renewable energy and energy efficiency, sustainable food production and diets, active transportation, and green cities will lower climate pollution while simultaneously reducing the incidence of communicable and non-communicable disease, improving mental health, and promising significant health care cost savings,” the Call to Action states.
Holistic Primary Care’s 2019 practitioner survey offers insight into our own readers’ views on environmental issues: 70% of respondents believe climate change is a pressing public health issue that must be addressed as such. Broken down by age, concern was somewhat higher among younger readers; 69% of those aged 30-40 years see climate change as requiring immediate attention, versus 58% of readers aged 51-60. But concern is high across the board.
 Elsewhere in the world, prestigious medical organizations are also joining the call for change. In June, the British Medical Association (BMA) agreed to formally declare a “climate emergency” and to campaign for carbon neutrality by 2030.
Elsewhere in the world, prestigious medical organizations are also joining the call for change. In June, the British Medical Association (BMA) agreed to formally declare a “climate emergency” and to campaign for carbon neutrality by 2030.
In September, the Australian Medical Association followed suit, asserting that “climate change is real and will have the earliest and most severe health consequences on vulnerable populations around the world.”
Disproportionate Impacts
That’s an important point. Climate change, environmental degradation, and deteriorating infrastructure ultimately threaten everyone. But they are having their strongest, most immediate impact in economically disadvantaged communities. Globally, the greatest damage is happening in poor “undeveloped” countries that are least responsible for climate pollution.
The Climate, Health and Equity Policy Action statement underscores this fact:
“Climate change exacerbates health inequities, disproportionately harming the most vulnerable among us—children and pregnant women, people with low income, the aged and people with disabilities and chronic illnesses, some communities of color, indigenous people and tribal communities, immigrants, marginalized people of all races and ethnicities, and outdoor workers.”
In part, the disproportionate impact is because poor people have less access to the political, economic, social, and environmental resources to cope with climate threats.
To use one example, wealthy people have insurance policies that enable them to rebuild their beachfront houses when they’re flooded. They often have—or can afford—other places to live, and their assets are protected. But poor people in lowland communities easily find themselves homeless with little recourse when a hurricane hits. The wealthy are not immune to the devastating blows of climate instability, but in general, they have more of a cushion.
In some regions, climate shifts are rendering vast regions unlivable. Dwindling access to clean water, drought, and famine are fueling forced migration and armed conflict, says Dr. Solomon.
State of Emergency
At the University of Washington’s Center for Health and the Global Environment (CHanGE), director Jeremy J. Hess, MD, MPH is working to  advance climate solutions in the medical world. He’s also, quite literally, shouting “emergency!”
advance climate solutions in the medical world. He’s also, quite literally, shouting “emergency!”
An ER physician at the University of Washington, he has a unique perspective on the issues.
“I see a lot of what’s coming down the pike is probably disproprortionately going to affect emergency medicine and the emergency medicine system,” Hess proposed, “So I feel it’s an important issue for our specialty.”
His research at CHanGE has led him to the conclusion that efforts to simply mitigate the effects of global warming are no longer enough. “We have moved into an area where we can’t just talk about avoiding dangerous climate change. It’s at our doorstep––and we need to start thinking about how to reduce risks more effectively for all sorts of different hazards.”
Extreme weather is disrupting health care delivery, access, and flow of supplies. Across the country, recent hurricanes, floods and wildfires have led to hospital closures, some lasting for weeks or months at a time.
Last year, Hurricane Maria destroyed manufacturing plants on Puerto Rico that produce pharmaceuticals, medical devices, and other basic supplies like IV saline bags for the US healthcare market. The impact was felt far beyond the island.
CHanGE does not sugar-coat the situation. The center’s website notes that heatwave related deaths are expected to increase tenfold over the next 40 years; that 86 children per hour die of undernutrition made worse by climate instability in key agricultural regions; that warming climates worldwide are expanding the range and prevalence of pathogen-bearing mosquitos, ticks, fleas, and rodents.
Chronic Inflammation
In the month of October 2019 alone, more than 185,000 acres of land in California—were destroyed by wildfire, according to the state’s  Department of Forestry and Fire Protection (CDFFP). The Getty Fire which destroyed more than 600 acres in Los Angeles, and the Kincaid Fire north of Santa Rosa burned through a staggering 77,758 acres, and took many days to contain. New fires can start on any given day.
Department of Forestry and Fire Protection (CDFFP). The Getty Fire which destroyed more than 600 acres in Los Angeles, and the Kincaid Fire north of Santa Rosa burned through a staggering 77,758 acres, and took many days to contain. New fires can start on any given day.
Wildfires are nothing new in the western states, just as hurricanes and floods have always been part of the picture in the south and along the coasts. But there’s no question that the frequency and severity are rising.
One could say that the southwest has a bad case of chronic inflammation: what was once an episodic threat has become a “new normal.”
CDFFP reports that the duration of fire season has increased by 75 days in recent years, starting earlier and ending later every year. More than 26 million California and Arizona residents now live under red flag warnings—a National Weather Service designation that indicates optimal conditions for wildfires.
“Climate change is considered a key driver of this trend. Warmer spring and summer temperatures, reduced snowpack, and earlier spring snowmelt create longer and more intense dry seasons that increase moisture stress on vegetation and make forests more susceptible,” the CDFFP website states.
Firefighters and first responders obviously face imminent health risks, but smoke inhalation is becoming the norm in many communities in the fire zones. Hospital and clinic evacuations are also part of the new reality. In late October, Sutter Health was forced to evacuate its Santa Rosa Regional Hospital and transfer more than 100 severely ill inpatients to other facilities.
Extreme fire seasons have forced California’s hospitals to step up their rapid response protocols. But CHanGE’s Dr. Hess says most of the nation’s medical systems are woefully unprepared for the onslaught on the horizon. Mitigation efforts are all well and good, but CHanGE is emphasizing “pandemic preparedness.”
Injustice to Children
Children are uniquely susceptible to the consequences of climate change. They’re inherently vulnerable to the immediate effects, and they will inherit the long-term consequences.
This is a big reason why so many teenagers, prompted by young activists like Greta Thunberg, Xiuhtezcatl Martinez, Jamie Margolin, and Xiye Bastida are striking school and taking to the streets.
The American Academy of Pediatrics (AAP) officially recognized climate change as a child health issue in 2015. That year, the AAP released a report detailing the link between climate change and illness in kids, asking “pediatricians and politicians to work together to solve this crisis and protect children from climate-related threats including natural disasters, heat stress, lower air quality, increased infections, and threats to food and water supplies.”
The report cites a WHO stat indicating that more than 88% of the burden of disease attributable to climate change occurs in children younger than 5 years old.
“Failure to take prompt, substantive action would be an act of injustice to all children,” the AAP states.
In their NEJM report, Solomon and LaRocque list childhood malnutrition and food insecurity, lost school days due to extreme weather events, severe anxiety and PTSD among the many negative effects of the climate crisis on children.
The Great (Political) Divide
In June 2019, Richard Carmona and David Satcher––two former US Surgeons General––echoed similar concerns in a New York Times opinion piece.
 “Climate change represents a profound threat to the public’s well-being,” the physicians wrote. “The country needs to understand the public health implications of a warming climate.”
“Climate change represents a profound threat to the public’s well-being,” the physicians wrote. “The country needs to understand the public health implications of a warming climate.”
Carmona and Satcher state the importance of securing a “safe climate and healthy atmosphere for all present and future generations.”
Politically, climate change is a highly partisan issue: According to polls by the Pew Research Center, 84% of Democratic voters view climate change as a “major threat,” up from 40% in 2013. Among Republican voters, the number is 27%. Pew puts the average across the nation at 57%.
Given that divide, the joint statement from Carmona and Satcher is an important symbolic gesture: the two served under very different administrations—Carmona under George W. Bush, and Satcher under Bill Clinton.
But symbolic gestures and pious position statements won’t avert climate disasters, nor do they impress the young people calling out for change.
As Greta Thunberg said dryly in her brief but powerful message during the New York City climate strike on September 20:
“Everywhere I’ve been the situation is, more or less, the same. The people in power, their beautiful words are the same. The number of politicians and celebrities who want to take selfies with us are the same. The empty promises are the same. The lies are the same. And the inaction is the same. Nowhere have I found anyone in power who dares to tell it like it is.”
Oil & the Juliana Generation
15-ton Brontosaurus in the room is, of course, the fossil fuel industry and its central role in the global economy.
No realistic discussion about mitigating climate change will go very far without banging into oil, coal, and the CO2 emitted when we burn them.
The Carmona-Satcher statement is notable for the fact that the former Surgeons General used their Times op-ed to express support for the “Juliana 21,” a group of young climate activists and their landmark constitutional climate lawsuit.
Kelsey Juliana––the named plaintiff in Juliana v. US––and 20 other youth from around the country, sued the federal government in 2015 over its  contributions to climate change, and its abject failure to keep children safe from its perils.
contributions to climate change, and its abject failure to keep children safe from its perils.
The suit, filed with the US District Court of Oregon alleges that the government has known about the role of fossil fuels and carbon emissions as drivers of global warming for over half a century––yet it continues to willingly promote and protect the interests of the fossil fuel industry at the public’s expense.
Juliana v. US is not the first suit of this kind. But it is the first to get a nod from a highly placed judge. In 2016, Judge Ann Aiken of the US District Court of Oregon stated that she supports the idea that access to a clean and life-sustaining environment is a basic human right—the core premise of the Juliana 21 case.
Not surprisingly, the federal government has tried repeatedly—but still unsuccessfully—to have Juliana v. US dismissed. Following a June 4th hearing at which oral arguments were presented, the Juliana group is currently awaiting a decision from the US Court of Appeals for the Ninth Circuit. As of this writing, the trial is currently on hold.
Regardless of one’s political leanings or interpretation of climate science, the burning of fossil fuels presents major immediate risks to humans and the environment.
 “Our dependence on fossil fuels has unequivocal health implications, right now––and completely separate from the greater climate implications,” says CHanGE’s Dr. Hess. “It’s not possible to suggest that fossil fuel combustion is not bad for peoples’ health––that’s incontrovertible. I would challenge anybody to interpret the evidence differently.”
“Our dependence on fossil fuels has unequivocal health implications, right now––and completely separate from the greater climate implications,” says CHanGE’s Dr. Hess. “It’s not possible to suggest that fossil fuel combustion is not bad for peoples’ health––that’s incontrovertible. I would challenge anybody to interpret the evidence differently.”
Going the Wrong Way
CO2 emissions from fossil fuel combustion were responsible for around 76% of the US total human-caused greenhouse gas emissions (GHG) in 2017, the US Energy Information Administration reported earlier this year.
In one of the more striking climate reports to date, the United Nations Intergovernmental Panel on Climate Change concluded late last year that global net GHG emissions must be cut to nearly 50 percent of 2010 levels by the year 2030 to avoid global warming’s most catastrophic consequences.
Unfortunately, energy use trends show that we’re moving in the opposite direction. For the second year in a row, worldwide CO2 emissions increased to an estimated record high of just over 37 billion tons in 2018, an increase of 2.7 percent over 2017 levels.
The Juliana complaint claims that the government’s inaction is not only unjust, but unconstitutional, violating “the youngest generation’s constitutional rights to life, liberty, and property.” It further charges the fed with failing to preserve “essential public trust resources,” says Our Children’s Trust, the nonprofit environmental advocacy group providing legal counsel to the youth plaintiffs.
Foul Weather Friends
Regardless of how the Juliana case is ultimately decided, it is a landmark in the climate remediation movement, one that has galvanized the attention of many medical professionals.
Earlier this year dozens of health professionals and organizations joined together to amplify the voices of the Juliana 21 by submitting an amicus curiae brief to the District Court. The report summarizes their collective observations as clinicians and researchers studying the harmful impacts of GHG emissions on people born in the United States since 1995—the so-called “Juliana Generation.”
“There is scientific consensus that GHG emissions are causing major physical, chemical, and ecological changes to the planet, manifesting as extreme weather events, including heat waves and heavy precipitation, as well as droughts,” the brief states.
“The medical community widely considers the health effects of human-induced climate change, GHG emissions, and the other air pollutants that are emitted when fossil fuels are combusted to be significant public health threats.”
Those threats are greatest among the youngest people. “This generation is suffering—and will continue to suffer as they age—harms different from those of prior generations,” the group wrote.
Healthcare’s Dirty Footprint
If healthcare is going to be a positive force in attenuating the climate disaster, it needs to clean up its own house.
 “I would argue that one thing we’re being a little disingenuous about as a profession is the impact of our activities, particularly energy use,” Dr. Hess told Holistic Primary Care. “Our carbon footprint in health care is quite high. We rely on all this energy that’s generated through fossil fuel combustion, and that has health implications.”
“I would argue that one thing we’re being a little disingenuous about as a profession is the impact of our activities, particularly energy use,” Dr. Hess told Holistic Primary Care. “Our carbon footprint in health care is quite high. We rely on all this energy that’s generated through fossil fuel combustion, and that has health implications.”
In their NEJM piece, Solomon and LaRocque note that the health care sector—which represents almost 18% of the GDP—is responsible for nearly one-tenth of all GHG emissions in the US. If it were its own country, it would “rank seventh in the quantity of such emissions internationally.”
According to Hess, the adverse health impact of energy use within the US health care sector “is of the same order of magnitude as harm caused by medical error, which of course we spend a tremendous amount of time trying to reduce.”
A recent article in Fortune magazine spotlights the massive amounts of non-recyclable waste generated by medical facilities. Aside from constantly consuming huge quantities of electricity and water, medicine relies heavily on single-use, disposable vinyl and plastic: gloves, syringes, IV bags, catheters, surgical instruments, lab equipment, medical devices….and all the plastic packaging that surrounds them.
As Fortune points out, if a hospital system gives flu shots to all of its 30,000 employees, it will run through roughly 1 metric ton of vinyl gloves—each pair used for perhaps 2-3 minutes.
Some health systems are taking steps to reduce their environmental impact. The authors of the Fortune piece cite Wisconsin-based Gundersen Health System as an example. The non-profit Gundersen is building geothermal walls and systems for methane capture from landfills, and  switching to wind-generated electricity and solar-powered hot water plumbing. They’ve yet to reach carbon neutrality, but Gundersen has cut its CO2, particulate, and mercury emissions by 80%.
switching to wind-generated electricity and solar-powered hot water plumbing. They’ve yet to reach carbon neutrality, but Gundersen has cut its CO2, particulate, and mercury emissions by 80%.
Other major systems including the Cleveland Clinic have also made major commitments to reducing their carbon emissions and non-recyclable waste.
For more than 20 years, Healthcare Without Harm—an independent non-profit group—has been working with clinics and hospitals in the US and abroad, to reduce their negative environmental impact. HCWH has been a major factor in the closure of more than 4,500 medical waste incinerators, in programs to phase out mercury in measuring devices, and in minimizing dependence on PVC-based medical supplies.
They offer a wealth of practical tips for improving the eco-profile of clinics large and small.
Physicians in private practice are well positioned to “green” their own practices, because they have control over their medical supplies and utilities. But practitioners working in larger facilities where they are not directly responsible for purchasing can still advocate for eco-friendlier approaches.
Clinicians can “talk to their operations staff and ask, ‘Where do swe get our electricity from? How do we make decisions about the options that are available to us? Could we be operating more consistently with our principles in terms of protecting peoples’ health?'”
 Medical professionals might also consider joining a health advocacy organization––Physicians for Social Responsibility and Health Care Without Harm are two examples––to gain tools for further developing their education and advocacy skills.
Medical professionals might also consider joining a health advocacy organization––Physicians for Social Responsibility and Health Care Without Harm are two examples––to gain tools for further developing their education and advocacy skills.
“It’s very helpful to be part of a community of people who you can network with, share resources and learn from,” said Amy Collins, MD, emergency medicine physician and Senior Clinical Advisor for Physician Engagement at Health Care Without Harm.
“I encourage people to join our network, get involved with the Medical Society Cosortium on Climate and Health, join a clinician climate action group, and just connect with other people––because you’ll be stronger in numbers, and you’ll also learn a lot from peers,” Collins urged.
For nurses, HCWH’s Nurses Climate Challenge, a program working to educate 50,000 nursing professionals by 2022, is a good place to start. To date, the program has engaged nearly 11,000 nurses.
Practitioners in larger health system might consider joining or creating a sustainability committee, or advocating to establish a “Medical Director of Sustainability” position if one doesn’t already exist.
Those interested in nutrition can work with food service departments to promote plant-based foods, develop rooftop gardens, on-site farmer’s markets, or CSA programs at their facilities. Educational events like HCWH’s annual CleanMed conference are also great ways to get involved in practical solutions.
Though the scope of the climate crisis is enormous, Collins believes physicians are among the most well poised to tackle it. “We are trusted, powerful messengers, especially health messengers––and we have an obligation to use our expertise and influence to advance climate solutions.”
END







